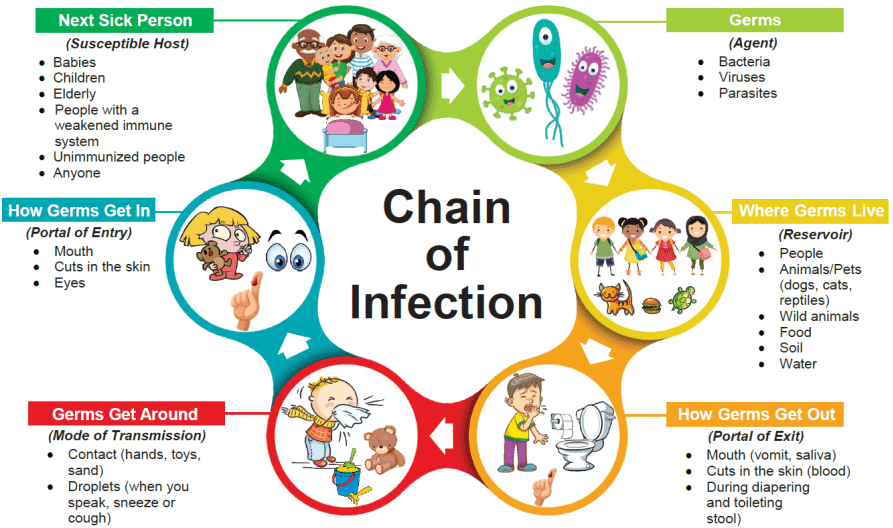
The chain of infection, if we think of it as an actual chain, is made up of six different links: pathogen (the infectious agent), reservoir, the portal of exit, means of transmission, the portal of entry, and the new host. Each link has a unique role in the chain, and each can be interrupted, or broken, through various means.
A series of events have to happen to enable germs (when we speak of germs in this section, this refers to bacteria, fungi, and viruses) to cause infections in a person. We call this the ‘Chain of Infection’. We can think of each part of the process as a separate ‘link’ in the chain. And if we can break a link at any part of the chain, we can stop infection arising.
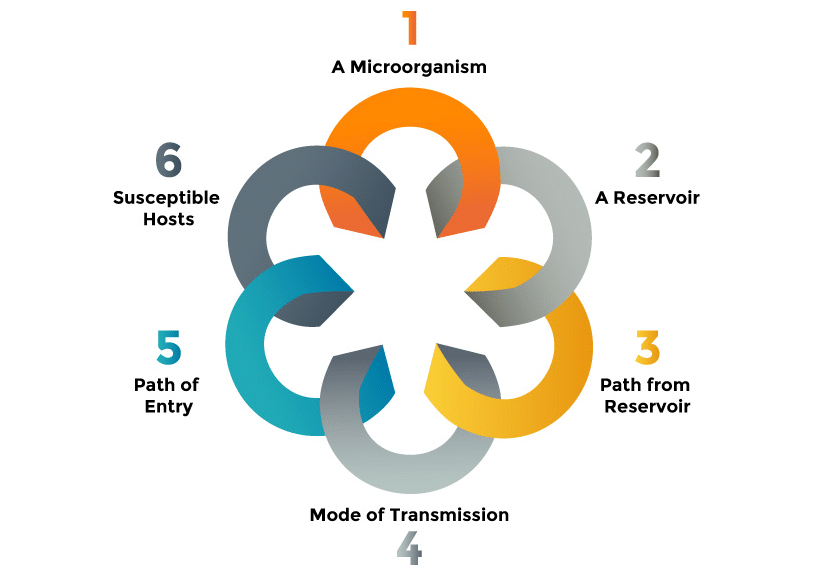
Links In The Chain
- The Organism: What is the organism? Bacteria, virus, protist, parasite, or fungi? The type of organism informs you of the types of disinfectants, antiseptics, and antimicrobials to use. Is it aerobic or anaerobic? What are its virulence factors? Toxin production in particular affects the course of the infection. What is its target host tissue?
- The Reservoir: Where do you find the organism in between outbreaks? What is the continual source of the infection? A reservoir can be environmental, the hospital setting or the water supply, or in a living organism, a rodent, bird, or even snail. Humans are the only reservoir for many human pathogens.
- Portal of Exit: How does the organism leave the reservoir? Does it leave in feces, blood, or mucus; in contaminated water; or in the blood meal of an insect.
- Transmission: How is the organism transmitted from one host to the next host? Does it need a living vector like a mosquito or flea? Some organisms like malaria have complicated life cycles involving more than one species. Can it be passed human to human? When passed human to human, it is transmitted by respiratory droplets, blood contact, semen, or other secretions? Is it transmitted on the hands of health care workers or the hospital ventilation system? Hand-to-mouth is a common mode for gastrointestinal pathogens.
- Portal of Entry: How does the organism enter the body? Does it come through inhalation, a break in the skin or mucus membrane, an insect bite, contaminated food? The portals of entry would be through the nose, skin, or mouth. Portal of entry tells you what type of personal protective equipment (PPE) to use to keep health care workers, family, and visitors safe.
Modes Of Transmission
An infectious agent may be transmitted from its natural reservoir to a susceptible host in different ways. There are different classifications for modes of transmission. Here is one classification:
- Direct
- Direct contact
- Droplet spread
- Indirect
- Airborne
- Vehicleborne
- Vectorborne (mechanical or biologic)
Indirect transmission, an infectious agent is transferred from a reservoir to a susceptible host by direct contact or droplet spread.
Direct contact occurs through skin-to-skin contact, kissing, and sexual intercourse. Direct contact also refers to contact with soil or vegetation harboring infectious organisms. Thus, infectious mononucleosis (“kissing disease”) and gonorrhea are spread from person to person by direct contact. Hookworm is spread by direct contact with contaminated soil.
Read Also: What Is Bass Clef Notes?
Droplet spread refers to spray with relatively large, short-range aerosols produced by sneezing, coughing, or even talking. Droplet spread is classified as direct because transmission is by direct spray over a few feet before the droplets fall to the ground. Pertussis and meningococcal infection are examples of diseases transmitted from an infectious patient to a susceptible host by droplet spread.
Breaking The Chain Of Infection
One of the basic infection control principles is the chain of infection. Transmission of infection in a hospital requires at least three elements: a source of infecting microorganisms, a susceptible host, and a means of transmission for bacteria and viruses.
“An example of the most simple chain of infection is an infected patient cared for by a healthcare worker (HCW) who doesn’t wash his or her hands before caring for another patient,” says Richard Wenzel, MD, MSc, of the Department of Internal Medicine of Virginia Commonwealth University in Richmond, Va. Wenzel adds that contaminated hands are one of the most likely means of transmission of bacteria in hospitals.
Read Also: Antiderivative Calculator – A Brief Introduction
“When you talk about the chain of infection, you must acknowledge Ignaz Semmelweis, who in the mid-1800s, noted how bacteria travel from caregiver to patient.” In a chapter on handwashing for A Guide to Infection Control in the Hospital, Wenzel describes how, as an obstetrician, Semmelweiss noticed the practice of physicians and medical students examining women who died of puerperal sepsis (later linked to infection by Streptococcus pyogenes) and then going directly to the wards where they examined women in labor. Wenzel writes, “Semmelweis noted that onwards where midwives delivered babies, few mothers died of puerperal sepsis. He knew that midwives did not witness autopsies. Semmelweis reasoned that something was carried from the autopsy room to the wards on the hands of physicians and students. He introduced a simple handwashing regimen and rates of death due to puerperal sepsis fell.”
Read Also: What Is A Hurdy Gurdy?